Peripheral arterial aneurysm is the dilatation of a peripheral artery due to weakness of its wall.
Most common arteries involved are the popliteal artery (behind the knee), the femoral artery (at the groin), the carotid and the lower extremity arteries (more rarely)
The main risk is peripheral embolization. In most aneurysms there is a significant amount of clot (thrombus). In some cases, a piece of clot can travel and block any peripheral vessel (peripheral embolization). A less common complication is rupture and bleeding.
Most patients do not have any symptoms. Some may feel a bulging mass at the site of the aneurysm. Others may have signs of ischemia. In popliteal or femoral artery aneurysms, patients may have leg pain during exercise or sleep, nonhealing ulcers or gangrene. Finally in carotid aneurysms they may experience temporary or permanent stroke.
The etiology of the aneurysm is unknown. Risk factor include age >60y, 1st degree relative with an aneurysm, high blood pressure or cholesterol and smoking.
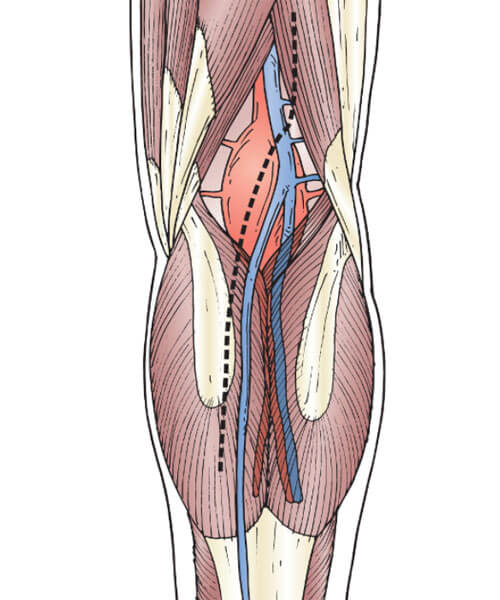
Popliteal Aneurysm
The diagnosis is confirmed with Duplex Ultrasound. If repair of the aneurysm is required, patients need to have a CT angiography or an MRI angiography.
The decision to repair the aneurysm is based on size, presence of thrombus or symptoms and age of the patient
There are two methods of treatment, minimally invasive (endovascular) and open surgical repair.
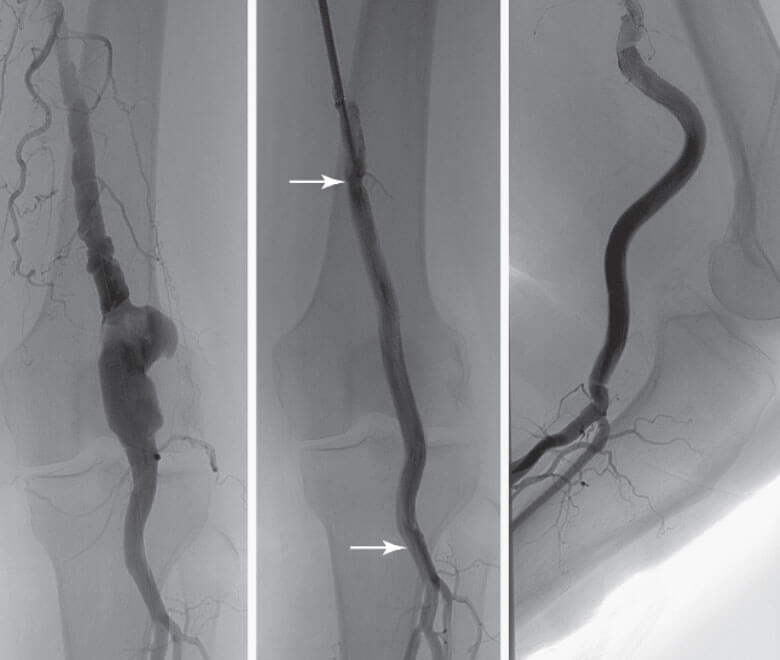
Endovascular Repair of Popliteal Aneurysm
During the minimally invasive procedure the repair of the aneurysm is performed from within the vessel (this is why it is called endovascular). Under local anesthesia, the vascular surgeon punctures the femoral artery of the leg and then places an endograft within the vessel. The patient is discharged in 1 day, there is no postoperative pain and recovery is very fast.
Open surgical repair requires general anesthesia and a large incision. The artery is replaced with a piece of patient’s vein or with a synthetic graft (more rarely). After the operation, the patient may be transferred to ICU for 1 day and he is discharged after one week. Full recovery requires 2 - 3 months.
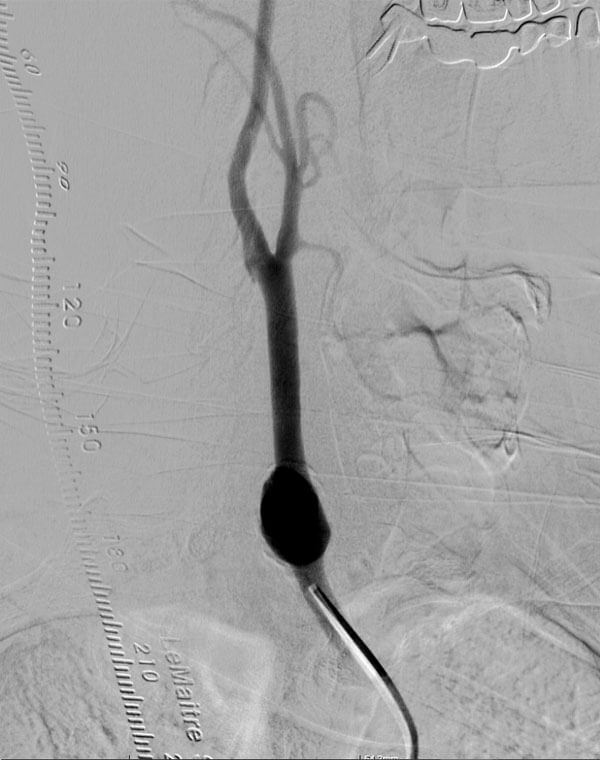
Carotid Aneurysm
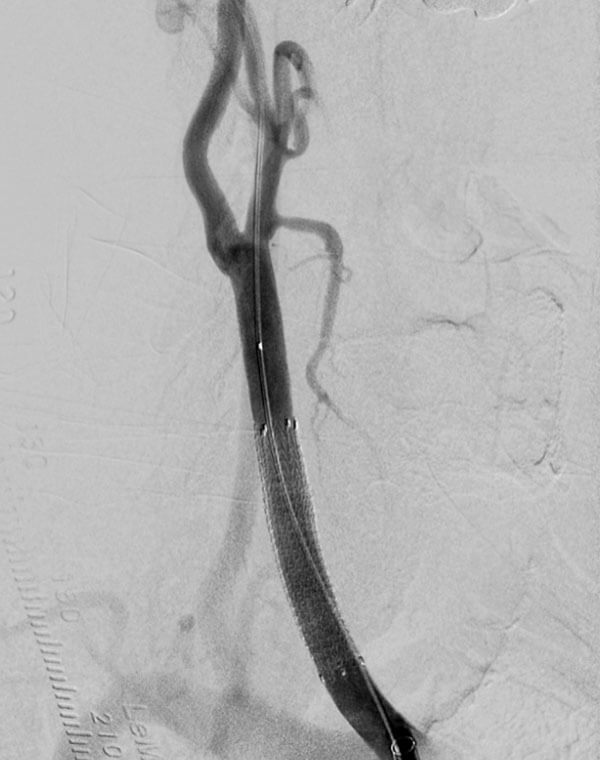
Endovascular Repair
The advantages of the minimally invasive procedure are obvious: no general anesthesia, no incision, no postoperative pain, early discharge and early recovery. The endovascular repair is performed in most but not all patients.
For both methods there are indications and contradictions.
The results of the endovascular repair are excellent when:
a) It is performed by experienced vascular surgeons in patients suitable for this technique.
b) It is performed in state of the art hybrid operating rooms which combine the safety of the operating room with the superb imaging capabilities of the angiography suite.
c) Last generation endovascular devices are used.
Patients with peripheral arterial aneurysm should consult vascular surgeons with experience in both endovascular and open surgical repairs in order to receive the most appropriate method of treatment.
